
Introduction
Healthcare organizations process thousands of documents every week: patient intake forms, insurance claims, referrals, lab reports, and discharge summaries. Most of this work is still done manually.
Physicians lose an average of 13 hours per week to documentation and order entry, while administrative staff spend another 7.3 hours on prior authorizations alone. That burden pulls clinical staff away from patients and stalls the revenue cycle.
Intelligent Document Processing (IDP) offers a practical solution by automating document capture, classification, extraction, and routing. This guide covers how IDP works in healthcare, where it delivers the most value, and what to evaluate before implementation.
TLDR:
- IDP uses AI to automatically read, classify, and extract data from medical documents replacing manual data entry
- Primary use cases include patient intake, referral processing, claims management, and medical records digitization
- Organizations see 40-50% faster processing, fewer claim denials, and improved staff productivity without headcount growth
- HIPAA compliance requires end-to-end encryption, role-based access controls, and built-in audit logging
What Is Intelligent Document Processing in Healthcare?
Intelligent Document Processing is an AI-powered technology that reads, classifies, and extracts structured data from medical documents including scanned forms, faxes, PDFs, and handwritten records then routes that data into downstream healthcare systems automatically.
IDP vs. Traditional OCR
Traditional OCR (Optical Character Recognition) converts document images into raw text, nothing more. IDP goes further: it understands document context, identifies specific fields like policy numbers and diagnosis codes, and validates extracted data against business rules before routing it to the right system.
| Capability | Traditional OCR | IDP |
|---|---|---|
| Text extraction | ✓ | ✓ |
| Document classification | ✗ | ✓ |
| Field-level data extraction | ✗ | ✓ |
| Validation against business rules | ✗ | ✓ |
| Automated system routing | ✗ | ✓ |
The Healthcare Document Challenge
That distinction matters because healthcare documents are unusually complex and varied. Organizations routinely handle:
- Patient intake and registration forms
- Referral and prior authorization requests
- Explanation of Benefits (EOBs)
- Lab reports and imaging results
- Discharge summaries
- Mixed fax packets containing multiple document types
The volume and quality inconsistency across these formats make manual processing unsustainable. While medical claim submissions are 98% electronic, 68% of medical attachments still move through fax or mail processed by hand. And with up to 80% of healthcare data remaining unstructured, the gap between what arrives and what systems can use is where delays, errors, and costs accumulate.
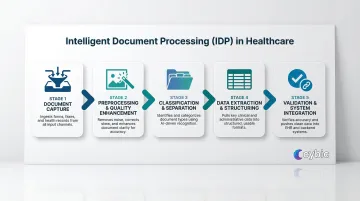
How IDP Works in Healthcare: Step-by-Step
1. Document Capture and Ingestion
IDP captures documents from all entry points automatically:
- Fax servers and email attachments
- Patient upload portals
- EHR exports and scanning systems
- Third-party provider submissions
Staff no longer manually route files the system ingests documents the moment they arrive.
2. Preprocessing and Quality Enhancement
Before extraction begins, IDP corrects common scan quality issues:
- Straightens skewed pages
- Enhances low-resolution images
- Removes background noise and artifacts
- Normalizes contrast and brightness
This preprocessing step directly determines downstream accuracy. Poor image quality causes extraction errors, so addressing it upfront improves the entire workflow.
3. Classification and Document Separation
A single incoming fax might contain a lab report, a referral, and an insurance card, all as one file. AI classification models separate these automatically, routing each document type to the correct processing pipeline without any manual sorting.
4. Data Extraction and Structuring
Extraction models identify and pull key fields:
- Patient demographics (name, date of birth, contact information)
- Insurance details (policy number, group ID, payer name)
- Clinical information (diagnosis codes, procedure codes, provider details)
- Financial data (payment amounts, claim numbers, denial reasons)
The system converts unstructured content into structured, usable data ready for downstream systems.
5. Validation, Exception Handling, and System Integration
Extracted data is validated against business rules:
- Patient ID must match existing records
- Policy numbers must follow expected formats
- Diagnosis codes must be valid ICD-10 codes
- Required fields must be present and complete
Low-confidence fields are flagged for human review. Staff only handle exceptions and not every document which keeps throughput high without sacrificing accuracy.
Validated data then flows directly into EHR, revenue cycle management (RCM), or enterprise content management (ECM) systems via API integrations, removing manual re-entry from the equation.
Key Use Cases of IDP in Healthcare
Patient Intake and Registration Automation
IDP reads registration forms and automatically updates patient records in the EHR, eliminating front desk data entry and reducing wait times at the point of intake. Staff can focus on patient interaction rather than keyboard work.
Referral Processing and Prior Authorization
IDP extracts diagnosis details, requested services, and clinical notes from referral and prior authorization forms, then routes structured data to scheduling or authorization teams. This reduces treatment delays caused by slow manual processing.
Transitioning to fully electronic prior authorization saves providers 14 minutes per transaction and reduces costs from $16.29 per manual transaction to $5.43 per electronic transaction. A 2025 study published in JAMA Network Open found that automation reduced median authorization times by 33.9% and cut denials by 65.4%.
Medical Billing and Claims Processing
IDP extracts claim fields such as procedure codes, patient information, payment details, denial reasons and feeds them directly into revenue cycle management systems. This accelerates the billing cycle and reduces claim rejections from data entry errors.
The financial stakes are significant. The national average claim denial rate sits at 12%, with most errors originating before the claim is ever submitted:
- 44% of denials come from front-end errors
- Registration and eligibility issues drive 24.33% of all denials
- Missing or invalid claim data accounts for another 15.89%
- Reworking a single denied claim costs providers an average of $57.23

Clean data at submission isn't just an efficiency goal, it directly protects revenue.
Medical Records Digitization and Chart Abstraction
IDP helps medical records teams index and digitize large document archives such as separating and classifying bundled clinical notes, lab results, and imaging summaries. This makes records searchable and accessible without manual sorting, supporting both clinical care and regulatory compliance.
Compliance and Audit Document Management
IDP automates the audit trail by recording every extraction, validation, and human review step. Each document carries a timestamped log showing who reviewed it, when, and what changes were made giving organizations the traceable records required for HIPAA compliance and regulatory inspections.
Key compliance capabilities IDP supports:
- Automated audit logs for every document interaction
- Timestamped human review records with user attribution
- Version tracking across extraction and validation steps
- Inspection-ready documentation without manual assembly
Benefits of IDP for Healthcare Organizations
Faster Processing and Reduced Turnaround
IDP processes documents in seconds rather than hours, removing the manual handoff delays that slow intake registration, referral scheduling, and claims submission. Healthcare organizations using AI document automation have reported approximately 50% reduction in administrative processing time. One implementation involving prescription processing achieved an 80% reduction in cycle time.
Improved Data Accuracy and Fewer Claim Rejections
AI extraction models read documents consistently, eliminating the transcription errors that cause claim denials, duplicate records, and billing disputes. Manual data entry in healthcare carries a 3.7% error rate, while AI-driven systems achieve field-level accuracy above 98%. Human review kicks in only for low-confidence extractions and not as a default step for every document.
Increased Staff Productivity Without Headcount Growth
Automating repetitive extraction tasks frees staff from data entry and redirects their time to higher-value work. Healthcare organizations can scale document volumes without adding administrative headcount. In practice, that shift looks like:
- Fewer staff hours spent keying in patient intake forms and referrals
- Faster exception resolution with human reviewers focused on flagged cases only
- More capacity for patient-facing activities and care coordination
Stronger Compliance Posture and Audit Readiness
Every document action is logge who reviewed it, when, and what was changed giving compliance teams a complete, timestamped trail. This directly supports HIPAA documentation requirements and eliminates the gaps that come with manual, untracked workflows.
The financial stakes are real: OCR enforcement has resulted in $144.8 million in HIPAA fines, frequently tied to inadequate access controls and missing audit trails.
Common Healthcare IDP Challenges and Compliance Considerations
Document Quality and Format Variability
Healthcare documents present real processing challenges:
- Handwritten notes and signatures
- Low-quality fax rescans with artifacts
- Mixed document packets with missing pages
- Inconsistent templates from different insurers and facilities
Modern IDP platforms address these through image preprocessing and continuous model retraining. The system learns to handle degraded inputs and adapt to template variations over time.
HIPAA Compliance and Data Security Requirements
Any IDP solution handling Protected Health Information (PHI) must meet strict requirements:
- End-to-end encryption of data in transit and at rest
- Role-based access controls (RBAC) limiting document and data access
- Full audit logging of all system activities
- Secure deployment model (cloud, hybrid, or on-premise) aligned with organizational data governance policies
The HIPAA Security Rule (45 CFR 164.312) mandates these technical safeguards. Governance needs to be embedded at the architectural level such as RBAC, encryption, auditability, and data use policies should be built into the system's foundation, not added as an afterthought once deployment is underway.
Model Drift and Long-Term Accuracy Maintenance
Document templates evolve insurers update forms, hospitals revise reporting layouts and IDP models require continuous retraining to maintain accuracy. Human-in-the-loop review serves a dual function: catching errors in real-time and feeding corrections back into the model to improve future performance.
Human-in-the-loop review serves a dual function: catching errors in real-time and feeding corrections back into the model to improve future performance. Effective drift management typically involves:
- Monitoring confidence scores to flag low-certainty extractions
- Routing flagged documents to human reviewers for validation
- Logging corrections to create labeled data for model updates
- Scheduling periodic retraining cycles tied to template change events
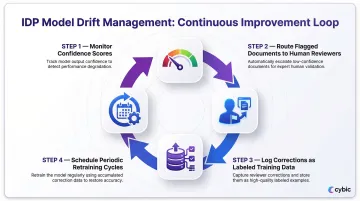
Addressing these challenges upfront such as quality variability, compliance, and model maintenance determines whether an IDP deployment delivers sustained accuracy or degrades quietly after go-live.
How to Evaluate and Implement an IDP Solution in Healthcare
Key Evaluation Criteria
Healthcare teams must assess several factors before selecting an IDP solution:
Extraction accuracy by document type - Demand metrics broken down by specific document categories (intake forms, referrals, claims, lab reports), not just overall averages.
Straight-through processing rates - What percentage of documents process end-to-end without human intervention?
Reviewer interface quality - How are low-confidence extractions surfaced to staff? Is the review workflow intuitive and efficient?
HIPAA compliance controls - Are encryption, RBAC, and audit logging embedded architecturally or added as afterthoughts?
HL7/FHIR standards support - Can the platform integrate with your EHR and RCM systems using healthcare data exchange standards? The CMS Interoperability and Patient Access Final Rule and subsequent mandates require FHIR-based APIs for prior authorization workflows by 2027.
Implementation Approach : Start Narrow, Then Scale
Follow this recommended rollout strategy:
- Begin with one high-volume, well-defined workflow - Patient intake or referral processing are ideal pilots
- Establish baseline metrics - Measure current processing time, accuracy rate, and exception volume before implementation
- Deploy and monitor - Track the same metrics post-implementation to quantify improvement
- Build internal confidence - Use early success to gain stakeholder buy-in before expanding to adjacent workflows
Choosing the Right Implementation Partner
Once your pilot is underway, the implementation partner you choose will determine whether IDP scales successfully or stalls. Look for a partner who brings:
- Deep familiarity with clinical workflows and healthcare data governance
- Demonstrated HIPAA compliance practices at the architectural level
- Experience integrating with EHR, RCM, and prior authorization systems
- Deployment flexibility across cloud, hybrid, and on-premise environments
Cybic's engineering-led model is built around this operational reality. Solutions integrate into existing healthcare infrastructure and compliance frameworks from day one, without requiring organizations to restructure around a new tool.
Frequently Asked Questions
What is intelligent document processing in healthcare?
IDP is an AI-driven system that automatically reads, classifies, and extracts data from healthcare documents replacing manual data entry across administrative and clinical workflows. It processes scanned forms, faxes, PDFs, and handwritten records, routing structured data directly into operational systems.
How does IDP differ from OCR in healthcare?
OCR converts document images to raw text, while IDP understands document structure, identifies specific data fields in context, validates extracted values, and integrates results into operational systems. IDP provides end-to-end automation, not just text conversion.
Is intelligent document processing HIPAA compliant?
Compliance depends on the solution's architecture. A HIPAA-ready IDP system requires end-to-end encryption, role-based access controls, full audit logging, and secure deployment options, all incorporated at the architectural level, not retrofitted after the fact.
What types of healthcare documents can IDP process?
IDP handles patient intake and registration forms, referrals, prior authorization requests, insurance claims, EOBs, lab reports, discharge summaries, and mixed fax packets.
How does IDP integrate with EHR and RCM systems?
Extracted, validated data flows into EHR, revenue cycle, and scheduling platforms via APIs and HL7/FHIR-compatible integrations, eliminating manual re-entry between document processing and downstream systems.
What is the best first use case for healthcare document automation?
Patient intake registration or referral processing are ideal pilots both are high-volume, well-defined workflows where automation delivers fast, measurable results and builds internal confidence for broader rollout. Many organizations see processing time cut by 50–70% within the first 90 days.